The DHIS2 Annual Conference takes place from 15-18 June 2026! Learn more
Research Round-Up: Extending and Strengthening Routine DHIS2 Surveillance Systems for COVID-19 Responses in Sierra Leone, Sri Lanka and Uganda.
A research article by Carl Kinkade, Scott Russpatrick, Rebecca Potter, Johan Saeboet et al. in the CDC EID Journal elaborates on how DHIS2 has been used to emplace more effective surveillance systems for COVID-19 using lessons from the Ebola outbreak.
The Ebola outbreak in 2014 prompted regional and global discussions around the establishment of multisectoral and integrated disease surveillance systems that can handle emerging healthcare challenges. The Global Health Security Agenda (GHSA), comprised of more than 70 countries, was established to strengthen disease surveillance and response by using real-time data to direct outbreaks prevention, detection and response. Following these discussions, many low- and middle-income countries committed to improving their national surveillance systems with the support of multilateral agencies including the Global Fund, Gavi and the World Bank. Additionally, funding from US agencies like PEPFAR, CDC and the PMI facilitated improvements to the core DHIS2 platform, which was already being used as a national HMIS platform or for surveillance purposes in most of these countries. These improvements included functionalities to generate predictive disease thresholds based on historical data and enable the creation of alerts via email, SMS and other means for more effective real-time notification.
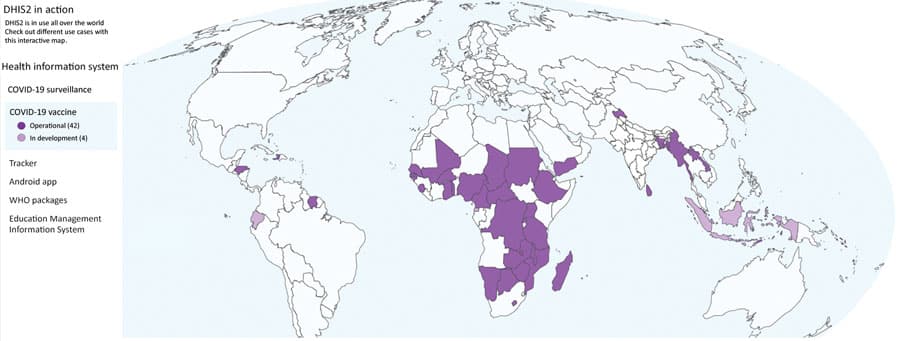
At the onset of the COVID-19 pandemic in 2019, 25 countries had adopted DHIS2 for national surveillance and implemented routine electronic reporting on priority diseases, aligned with the WHO AFRO Integrated Disease Surveillance and Response (IDSR) strategy. The number of countries using the DHIS2 platform for COVID-19 surveillance quickly grew to about 55 in 2020 following the pandemic. DHIS2 proved valuable as an efficient electronic tool for health information management with disaggregated data access from the lowest organizational unit to policy-making levels. The successful scale-up of DHIS2 for COVID-19 surveillance and emergency response is attributed in part to three key factors:
- Flexible, extendable open-source technology that enables local innovation.
- An inclusive and participatory global community of practice to share knowledge and approaches between countries and regions.
- Long-term investments in local capacity to design and manage the system, with full autonomy over the system by Government actors.
This study describes how prior investments in DHIS2-based surveillance systems in Sri Lanka, Sierra Leone, and Uganda enabled each country to rapidly respond and adapt their existing DHIS2 systems to meet the needs of the COVID-19 pandemic.
Sierra Leone: Having used DHIS2 for HMIS since 2008, Sierra Leone integrated electronic reporting of disease data at the facility level in line with WHO’s IDSR framework. Weekly electronic reporting on 26 priority diseases started in 2016 and was extended to the whole country by 2019 with the support of the CDC, WHO and e-Health Africa. The country also developed an electronic case-based disease surveillance (eCBDS) system building on the HMIS infrastructure. These systems were modified in Sierra Leone during the COVID-19 outbreak by incorporating the WHO-recommended variables into the existing designs supporting acute respiratory illness surveillance. Key to this success was the institutionalization of the DHIS2 platform for disease surveillance and coordinated plans for scaling up the system across the entire country.
Sri Lanka: With significant local capacity developed over the decade-long use of DHIS2 for various health programs in the country, Sri Lanka was able to modify a DHIS2 instance in 2 days, to register all international travelers arriving in the country and monitor them for COVID-19 symptoms. This helped the country put in place an effective point-of-entry (POE) COVID screening by early February 2020. Sri Lankan authorities also engaged developers via a hackathon to work with a DHIS2 core developer, seconded to the country by UiO, to extend and integrate the platform for case reporting and nationwide surveillance. In 2 weeks, the team created innovative solutions and custom applications for contact tracing, analytics and an interoperability layer for data exchange with the country’s immigration information system. The team also implemented systems to identify available hospital intensive care beds by tracking bed occupancy in designated facilities. Sri Lanka further extended its COVID-19 DHIS2 system by including a national-scale electronic immunization registry for COVID vaccination. The system, through the interoperability layer, leverages the DIVOC platform to generate secure and verifiable vaccine certificates. As of December 2021, over 19 million persons have been enrolled in the registry. The Sri Lanka case study demonstrates how local capacity, governance and innovation allow countries to rapidly adapt and respond to needs, with limited reliance on interventions from outside partners to execute new designs.
Uganda: Uganda implemented a DHIS2-based eIDSR in 2013 for case-based reporting and collection of laboratory data for priority diseases. This early investment informed the development of a more generic case-based surveillance design framework approved by the WHO for vaccine-preventable disease reporting. This design served as the basis for COVID-19 surveillance packages and tools developed by UiO. Being an important logistics and transportation hub for Central Africa, the risk of rapid transnational spread of the virus was significantly higher. To avoid a crippling halt of essential commodities’ transportation and sustain adequate surveillance of COVID-19, HISP Uganda developed a new POE module within the eIDSR to screen people at all formal borders. Travelers’ data are collected using the DHIS2 Android Capture app and rapid tests conducted at the borders. Individuals with negative test results were issued with a printed pass containing the travelers’ passport photos and a QR code for verification. This allowed Uganda to maintain open borders critical for trade and economy during the height of the pandemic.
These local innovations have inspired global efforts to share best-practice configurations and make them accessible to the larger DHIS2 global community to accelerate uptake in additional countries. For example, the POE module developed by HISP Sri Lanka, along with configurations for contact tracing, reporting and dashboards, was packaged by UiO to create the COVID-19 case-based surveillance module to help other countries bootstrap similar implementations. These case studies demonstrate that entirely new platforms, systems and tools are not necessarily needed or effective in a public health emergency. Rather, adaptation and local innovation leveraging existing surveillance infrastructure and capacities for routine surveillance in countries, such as DHIS2, was shown to be an effective strategy for setting up digital systems to address emerging, novel disease threats.
Authors: Carl Kinkade, Scott Russpatrick, Rebecca Potter, Johan Saeboet et al.
Publishers: doi.org
Date of Publication: 02 November, 2022.
Link: https://wwwnc.cdc.gov/eid/article/28/13/22-0711_article